Preventive & Diagnostic Services
Comprehensive Oral Evaluation
We recommend an oral evaluation every 6 months starting no later than age 1. Our priority is PREVENTION and the overall health of your child. Research shows that the dental costs for children who have their first dental visit before age 1 are 40% lower in the first 5 years than for those who do not see a dentist prior to their first birthday.
Regular dental visits and establishing a “Dental Home” for your child can prevent problems from occurring or can diagnose and treat existing problems before they become serious and help return your child to ideal health. A Pediatric Dentist has at least two additional years of training beyond the four-year Dental School program. The additional training that Pediatric Dentist’s receive focus on advanced behavior management skills and techniques unique to children and those with special needs, dental restorative considerations and methods specific to the primary (baby) and developing permanent dentition, guidance of the growth and development of the face, jaws, teeth, and TMJ through interceptive and full orthodontics as well as training in Hospital Dentistry. A Pediatric Dentist, the staff, and even the office décor are specially trained and equipped to care for your child beginning in infancy through the teenage years.
In fact, kids of all ages have a lot of fun with us and tell us all the time how much they look forward to coming back to their next appointment.

Growth and Development Evaluation

Pediatric Dental specialists are the experts in the field of your child’s oral-facial growth and development. One of our jobs to make sure your child is on the right growth track and that their teeth, face, jaws, and airways (known collectively as the CRANIO-FACIAL STRUCTURES) are growing to their “best genetic potential”.
WHY?
The answer is that Craniofacial Growth is 90% to 95% complete by age 12 – so most of the craniofacial formation (or deformation) occurs by 12 years of age and after that, it becomes more difficult to guide or alter. Unfortunately, age 12 is still the average age that orthodontic and orthopedic treatment starts for most children worldwide. THIS MUST CHANGE – because waiting this long means we lose our chance to take advantage of the body’s inherent GROWTH POTENTIAL to help us. Waiting too long can often mean you are too late to make an effective change without settling for compromise or needing more complicated treatment.
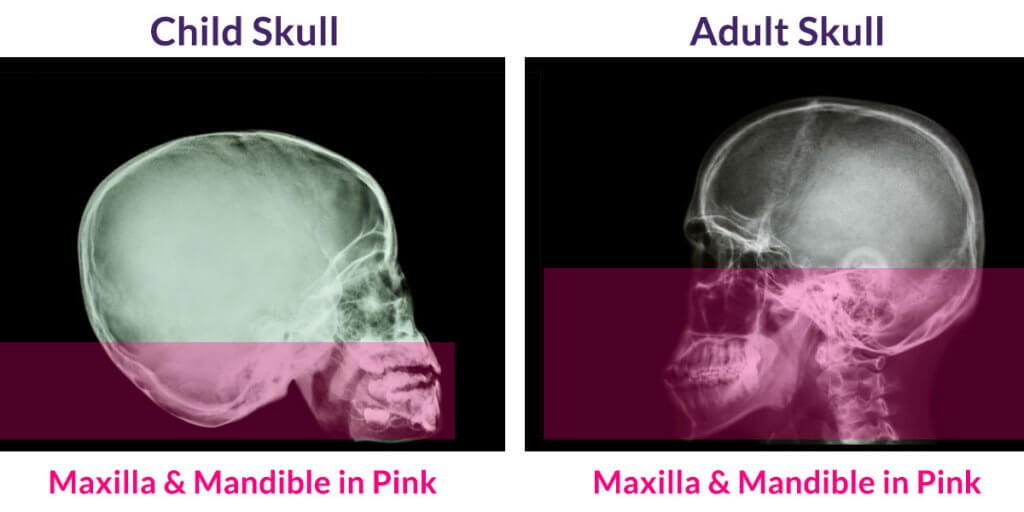
The maxilla (upper jaw) and mandible (lower jaw) are nearly 50% FORMED AT BIRTH AND ABOUT 90% GROWN BY AGE 12. Therefore, about 80% of craniofacial growth occurs between birth and age 12. After age 12, only a fraction of post-birth craniofacial growth remains.
Notice how much the bones that make up the mid and lower face, including the upper jaw (maxilla) and lower jaw (mandible), grow from birth to the end of puberty. We do not want to miss this crucial time of growth. Notice that in “normal development,” how much the mid and lower face (the maxilla and mandible) grow and how much they grow forward compared to the size of the cranium.
Dentists that understand Oral Facial Growth and Development are in a unique position to screen children for the recognizable signs and symptoms of mouth breathing, malocclusion, craniofacial anomalies and many related health conditions, such as Obstructive Sleep Apnea syndrome. Early diagnosis of airway obstruction, chronic mouth breathing, and malocclusion, along with identification of the underlying causes, is essential to prevent and/or help reverse oral-facial growth problems. The earlier problems with growth and/or underlying issues are detected, the more effective, the more simple and the less invasive treatment can be. Diagnosis of dental malocclusions and skeletal deformities associated with mouth breathing require comprehensive and frequent orthodontic examinations by dentists that have an understanding airway anatomy and physiology.
All infants should be screened for craniofacial growth issues that can affect airway form and function. Breastfeeding should be encouraged as it promotes nasal breathing, the development of proper swallowing patterns and decreases the incidence of mouth breathing. The reverse is true of bottle-fed infants. We realize that not all infants are breastfed for a variety of understandable reasons, but infants who are solely bottle fed should be screened more often for the subtle effects of mouth breathing, abnormal tongue swallowing patterns, tongue thrusting and palatal (upper) arch narrowing.
At the age of 2 and 3, subtle dental signs of nasal obstruction and mouth breathing can be seen.
From ages 3 to 12, early airway obstruction and craniofacial deformations often magnify themselves to such an extent that as time goes on, the problems can get more difficult and complicated to fix.
Role of Parents in Kid’s Oral Hygiene
Parents should lead and/or supervise their children’s tooth brushing for the first 12 years since every child will have unique motor functions, abilities and motivation levels. It is normal and expected that babies and young children often “do not like” to have their parents brush their teeth and many want to “do it themselves.” Although it’s OK to “take-turns” brushing, in order to properly remove plaque from the teeth and gum line area, an adult will have to do it. More often than not, this may require getting down on the floor or on a bed/sofa and placing the child’s head in your lap in order to “see” what you are doing. You may even need a “helper” to help you hold your child to get the job completed.
Brushing
It is NORMAL for your child to cry, but think of it as an opportunity to “better see the teeth” because the mouth is usually WIDE OPEN when crying. Even though it may break your heart to see or to make your little one cry – you are doing a very good thing by helping your child remain healthy and preventing tooth decay. The small periods of crying are worth your child not having tooth pain or the need for dental work in the future! If your child dislikes getting their teeth brushed, just imagine how much they will dislike having dental work done! In the long run, the effort you put into PREVENTION is more than worth it. Think of it like this: babies and young children cry when we do lots of things for their health and safety, such as “buckling the car seat” or making them “hold your hand” instead of running ahead; even changing their diaper can make a young child upset especially if they much rather be doing something else “more fun!”
Have a routine, stay persistent and strong and know that an ounce of prevention is better than a pound of disease.
At the age of around 6 years, most children are able to brush their teeth using a proper brushing technique, but they still need help; each time the child has finished brushing, parents should re-brush the hard-to-clean areas or at least “check” or “watch” them brush.
Between the ages of 6-12, the new ADULT/PERMANENT molars start to erupt, making parental supervision and assistance very important to make sure these often hard to reach teeth are properly cared for.
Toothpaste
The American Academy of Pediatric Dentistry (AAPD) recommends using fluoride toothpaste during brushing as soon as the first baby tooth erupts. But the amount of toothpaste needed is much less than you think, only about the size of a small grain of rice.
Infants and young children do not “spit” very well, but it’s OK if they do swallow a little bit as long as you follow this guideline. When children do learn to “spit,” then they can then use a “pea-sized” amount of fluoride toothpaste. IT IS IMPORTANT FOR AN ADULT TO ALWAYS APPLY THE TOOTHPASTE TO THE TOOTHBRUSH FOR THE CHILD SO THEY DO NOT USE TOO MUCH – like any other over-the-counter medicine or vitamin that is FLAVORED for CHILDREN, it “tastes good”, so keep it out of the reach of small children.
Flossing
The general rule is that if your child’s teeth “touch” together, they should be flossed. We recommend using “flossers” with younger children, as they can be a bit easier for a parent to manage than “string floss.” Try to make a game out of it by saying you are “playing Hide n’ Seek with any ‘Sugar Bugs’ the toothbrush may have missed.”
Nutrition
Feeding your child, a nutritious and healthy diet that is low in sugars, processed and highly refined foods is very important to prevent dental disease and foster good overall health – at any age! We can offer ideas and suggestions s for healthy eating at every stage of your child’s life.
It is important to note that the single most common CAUSE of dental decay is the FREQUENCY with which sugar-containing foods and drinks (anything other than water) that are in contact with the teeth, especially in-between meals.

Any drink that has sugar or is “sweetened” and consumed often and in-between meals will cause cavities – even if you brush your teeth. This includes: 100% juice, juice that is watered-down or “cut” with water, milk/chocolate milk (including milk alternatives like soy, almond, rice, hemp), tea, lemonade, sports drinks, flavored waters (look for ANY added sugars including honey, agave, fructose, corn syrup). Plain water is the ONLY drink that does not have the potential to cause cavities. If you are looking for variety, seltzer (fizzy) water or flavored waters that ARE NOT SWEETENED (you will have to read the label) can be a good choice. Try to avoid using sugar-free substitutes. They are not healthy alternatives as most are made from chemicals and they are “sweeter tasting” than natural sugar which can result in make the “craving” for sugar worse. Choosing a natural sweeter like Stevia is a better option, but remember anything sweet should be in moderation. On the limited and special occasions when your child does get something sweet to eat or drink, following it up with PLAIN WATER to rinse the mouth afterwards is RECOMMENDED.

It is also important to offer your child a variety of foods they can chew so that they can exercise their jaw muscles and so that they experience different textures of foods. Although convenient and non-messy, foods that are in pouches and food that dissolve in the mouth (like snacks that are “puffed” or melt in the mouth) should be only a small part of your child’s diet. Eating harder foods with various textures strengthens the oral muscles and jaw bones. Harder foods also assist with natural cleansing of the teeth.
Flouride
Anytime the Centers for Disease Control and Prevention (CDC) issues a statement saying that fluoride and fluoridation in dentistry is one of the 10 most important public health measures of the 20th century, you can rest assured there has been exhaustive evidence from years of research backing it up. You can read more about Fluoridation Facts here.
Fluoride is often called nature’s cavity fighter and for good reason. Fluoride, a naturally-occurring mineral, helps prevent cavities in children and adults by making the outer surface of your teeth (enamel) more resistant to the acid attacks that cause tooth decay and can promote “healing” or remineralization of the tooth surface.
Here Is How Fluoride Works to Benefit Your Child’s Teeth:
Before teeth break through the gums, the fluoride taken in from foods, beverages, and dietary supplements makes tooth enamel (the hard surface of the tooth) stronger, making it easier to resist tooth decay. This provides what is called a “systemic” benefit.
After teeth erupt, fluoride helps rebuild (remineralize) weakened tooth enamel and reverses early signs of tooth decay. When you brush your teeth with fluoride toothpaste or use other fluoride dental products, the fluoride is applied to the surface of your teeth. This provides what is called a “topical” benefit.
In addition, the fluoride you take in from foods and beverages and fluoride drops/tablets continue to provide a topical benefit because it becomes part of your saliva, constantly bathing the teeth with tiny amounts of fluoride that help rebuild weakened tooth enamel.
Berkshire County, MA does NOT have a water fluoridation program, meaning that there is NO fluoride in the public water system. If you live in a surrounding area that does have a water fluoridation program, but have WELL WATER, in general there is not enough naturally occurring fluoride contained in the ground to fluoridate the well water to an effective amount. Children that live in a non-fluoridated area or have well-water should be prescribed fluoride drops or tablets.
Digital Imaging (X-Rays)
We are proud to offer digital x-rays to our patients. There are many advantages of using digital x-ray technology including lower radiation exposure to the patient as compared to “regular film” x-rays. Additionally, using digital x-ray technology is better for the environment because they do not require “disposal” and management of lead film packaging or the harsh developing chemicals that are required for “film” x-rays.
We are often asked “Does my child really need an x-ray?” or “Are x-rays necessary?” The reason we need to take x-rays of your child’s mouth is that they are necessary in order to get accurate diagnostic information. Many diseases of the oral cavity (which includes the teeth and bone) cannot be seen or visualized with the eye and therefore cannot be diagnosed accurately or at all.
We use x-rays as a diagnostic tool to screen your child for any developmental defects: dental cavities, the presence of infections, some types of tumors, the effects of trauma, the health of your child’s airway, the position of unerupted teeth, any teeth that may be missing, developing incorrectly or headed in the wrong path (ectopic eruption), the presence of “wisdom teeth” or any additional (extra) teeth that may be present. Without this vital information, we cannot “see” from just looking with our eyes what is going on with your child’s dental health and development.
ARE DENTAL X-RAYS SAFE?
Dental x-rays are one of the lowest radiation dose studies performed in health care. A routine dental exam for an older child with all their permanent teeth, which includes 4 “bite-wings” is about 0.005 mSv, which is less than one day of natural background radiation. It is also about the same amount of radiation exposure from a short airplane flight (~1-2 hrs). We adhere to the ADA’s (American Academy of Dentistry) guiding principal called ALARA (As Low As Reasonably Achievable) regarding responsible radiologic practice, which states that, even once it’s been determined that x-rays are necessary, they should be as minimal as possible to reduce a patient’s exposure.
In general, we recommend taking your child’s first dental x-rays (2 “bite-wing” xrays) as soon as the back-baby teeth are “touching” together. At that time, we also usually also take 1 “occlusal” x-ray of your child’s front teeth to check the status of the developing permanent front teeth. We always take into consideration your child’s dental development, spacing of the teeth, “risk” factors for getting cavities and cooperation level; but on average, we take first set of x-rays at about 4 ½ years of age.
We also recommend taking your child’s first Growth and Development x-ray, either a 2-D Panoramic or 3-D scan (i-Cat® Technology) around the age of 7 or depending on the needs of your child.
We are always happy to have a discussion with you about your child’s need for x-rays, how often we take them and we will work hard to make you and your child comfortable. Since we practice according to the American Academy of Pediatric Dentistry (AAPD) and the American Dental Society (ADA) guidelines on x-ray use and periodicity, we do require that diagnostic x-rays be taken at the appropriate times and intervals for your child.
Dental Sealants
Brushing and flossing and a low sugar diet are the best ways to help prevent cavities. Still, it’s not always easy to clean every nook and cranny of your teeth – especially those back teeth you use to chew (called molars). Molars have deep grooves and uneven surfaces and a favorite place for leftover food and cavity causing bacteria to hide.
However, there’s a preventative “safety-net” that we offer to help keep those important 1st and 2nd molar teeth (also known as the “6 and 12 year molars”) healthy. It’s called a “sealant,” a thin, protective coating that adheres to the chewing surface of your back teeth. Sealants are no substitute for good oral hygiene habits and healthy eating, but they can keep cavities from forming and may even stop early stages of decay from becoming a full-blown cavity.
In fact, sealants have been shown to reduce the risk of decay by nearly 80% in molars. This is especially important when it comes to your child’s dental health. In October 2016, the Centers for Disease Control released a report on the importance of sealants for school-aged children, of which only 43% of children ages 6-11 have. According to the CDC, “school-age children without sealants have almost three times more cavities than children with sealants.”